Have your nails changed color, lost their shine, become brittle and disintegrated, or even fallen off your nails?It is probably about onychomycosis, that is, fungus, an insidious disease that is very difficult to treat and often recurs, especially if you delay visiting a doctor.Which doctor treats toenail fungus and what does proper onychomycosis treatment look like?
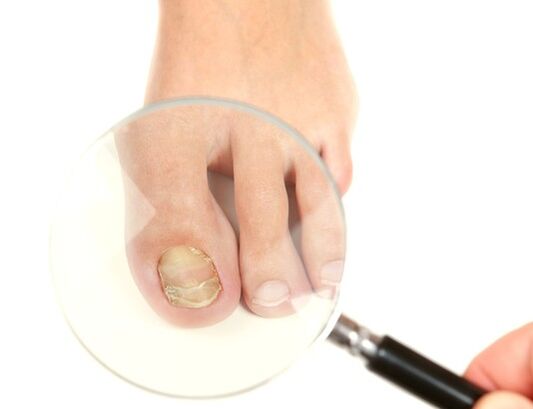
Types of nail fungus and symptoms
Fungal infections account for up to 15-40% of all nail diseases.The most common causative agents are trichophytons - parasitic fungi, and somewhat less often - candida - yeast fungi.Risk factors are:
- masculine gender;
- increased sweating of the feet;
- nail injuries;
- visiting public baths and swimming pools;
- immunosuppression due to diabetes mellitus and HIV infection, long-term use of corticosteroids;
- wearing synthetic socks and shoes made of unnatural materials.

The clinical manifestations of nail fungus are different.Taking this into account, modern medicine identifies six main forms:
- White superficial - initially the surface layers of the nail plate are affected, and then the degenerative process spreads deep into the tissues.Most often, this variety appears as white lesions that crumble;less often, there may be white lines.
- Normotrophic - the thickness and shine of the nail remain the same, the plate only changes color, and white and yellow spots and stripes appear.
- Hypertrophic - the nail constantly thickens and deforms due to the active division of skin cells located under the nail plate.
- Atrophic - the nail becomes gray-brown, while its thickness constantly decreases, due to which the nail can be completely exposed.
- Proximal – quite rare.The lesion affects the fold of the nail, while the final parts of the nail remain intact for a long time, i.e. undamaged.
- Total - the entire nail plate is involved in the pathological process and often develops against the background of reduced immunity.
Second medical opinion
Experts from leading Russian and foreign medical institutions will give their opinion on the results of tests and examinations, comment on the previously established diagnosis and prescribed treatment.
"In onychomycosis, the nail plate often loses its connection to the dermis, so it can easily be removed accidentally or intentionally. Doctors call this condition onycholysis."
Which specialist should I contact?
Which doctor treats nail fungus?In most cases, a dermatologist will help solve this problem.The doctor will conduct an objective examination and laboratory tests to determine the cause of the patient's dystrophic nail lesion.Only after that, appropriate drug therapy is selected.
In complex clinical cases, the help of a more specialized specialist - a mycologist - is needed.This is a doctor of dermatology who deals exclusively with fungal diseases of the skin, hair and nails.
"If you don't know which doctor treats nail fungus, make an appointment with a dermatologist. This is usually enough to establish a diagnosis and start timely therapy."
Diagnostic methods
If there are suspicious signs, such as changes in the shape and thickness of the nail, suspicious spots and stripes, crumbling, the doctor must conduct laboratory diagnostics before prescribing treatment.For this purpose, the changed nail plate is collected - a part is carefully cut off with special tweezers.The obtained biomaterial is subjected to:
- microscopic examination - results are obtained almost immediately, as fungal spores and mycelium are clearly visible under a microscope;
- cultural research - the results are evaluated only after 0.5-1.5 months, during which time the fungi grow and form colonies.This method allows you to identify the type of causative agent, as well as assess its sensitivity to antifungal drugs.
"Polymerase chain reaction - the creation of multiple copies of a single piece of DNA - is used only in difficult diagnostic cases when culture cannot determine the type of causative fungus."

Therapy
It is important to know which doctor to consult for nail fungus, because delayed treatment is not only a cosmetic problem, but also a medical one.Onychomycosis has been shown to increase the risk of the following conditions:
- pain and discomfort in the legs;
- difficulty walking and wearing shoes;
- discord in the professional and personal spheres of life;
- generalization of fungal infection on the skin of the legs and hands, groin;
- infection of other family members;
- increased sensitivity of the body to fungal antigens with the development of bronchial asthma and atopic dermatitis;
- bacterial infections of the skin - fungi disrupt the integrity of the dermis, and pathogenic and conditionally pathogenic bacteria easily enter the resulting microcracks.
Therefore, treatment is necessary in all cases of diagnosed nail fungus.Therapy is divided into two types:
- Local antifungal - the drug is applied directly to the nail plate.
- Systemic antifungal - the drug is taken orally, and the bloodstream reaches the "problem" site.

Currently, combined treatment is used for onychomycosis, when local application of a drug (medical nail polish or cream) is combined with drugs.Local monotherapy is less effective because keratin and closely adjacent epithelial scales prevent drug penetration into the nail plate.Thus, the concentration of the active component can be reduced by a thousand times.Therefore, local therapy is possible only in the initial phase of superficial nail damage and in the presence of contraindications to systemic antifungal drugs.
"If one family member is diagnosed with nail fungus, the whole family is treated at the same time, because onychomycosis is a particularly contagious disease."
After the course of treatment, the doctor must prescribe control tests - microscopy of the nail plate.If there are no fungi in the biomaterial, the person is considered to have fully recovered.In the future, it is important to follow the rules of prevention to avoid re-infection:
- use safety shoes when visiting hotels, gyms, public baths and swimming pools;
- apply antifungal powders and adsorbents to the foot - according to indications;
- wear socks made of natural fabrics;
- trim your nails regularly using individual pedicure accessories;
- replace old shoes with new ones, as they may contain a large number of dangerous fungi.

A simple rule: the earlier treatment is started, the more effective it is - in the case of onychomycosis, it works more than ever.Therefore, do not delay the visit to the doctor if you notice that the appearance of your nail has changed.
Which doctor should I consult for toenail fungus?
If you suspect onychomycosis, you should seek help, for example from a general practitioner.The doctor will prescribe tests, after which he will make a diagnosis and give a referral to a specialist.
















